Medical Disclaimer: This content is for informational purposes only and does not constitute medical advice. Insulin resistance, pre-diabetes, and metabolic syndrome are medical conditions requiring professional diagnosis and management. Please consult a qualified healthcare provider, endocrinologist, or registered dietitian before making significant dietary changes, especially if you are taking glucose-lowering medications.
Vegan Diet for Insulin Resistance: The Complete Plant-Based Metabolic Health Guide
TL;DR
A vegan diet for insulin resistance is one of the most powerful dietary interventions available for restoring metabolic health. Plant-based diets improve insulin sensitivity through five distinct mechanisms: high soluble fiber slowing glucose absorption, resistant starch feeding butyrate-producing gut bacteria that improve insulin signalling, plant polyphenols activating AMPK (the metabolic master switch), low saturated fat intake reducing intramyocellular lipid accumulation that causes insulin resistance at the cellular level, and caloric restriction through high-fiber food volume satiety. Clinical studies show plant-based dietary interventions can reduce HbA1c by 0.4-1.2% and improve HOMA-IR (insulin resistance index) by 20-30% within 12-16 weeks. This guide covers the four stages of insulin resistance, the plant-based reversal mechanisms, eight spotlight foods, a glycaemic index versus load chart, the three dietary tools, meal timing, and the 7-step daily protocol.
The Four Stages: From Insulin Sensitivity to Diabetes
A vegan diet for insulin resistance must begin with a clear understanding of what insulin resistance actually is and where it sits on the metabolic continuum. Most people are diagnosed only at the diabetes stage, missing years of opportunity for dietary reversal during the earlier, fully reversible stages.
The Four Metabolic Stages
Stages 2 and 3 are the primary target of a vegan diet for insulin resistance. Both are fully reversible with dietary intervention. The window of dietary reversal is wider and the results more dramatic than most people realise. A 12-16 week commitment to the dietary protocol in this guide produces measurable metabolic improvement at any stage short of advanced type 2 diabetes.

Ultimate 28-Day Vegan Meal Plan,
Easy Grocery List + 40 Recipes
• Comprehensive Guide
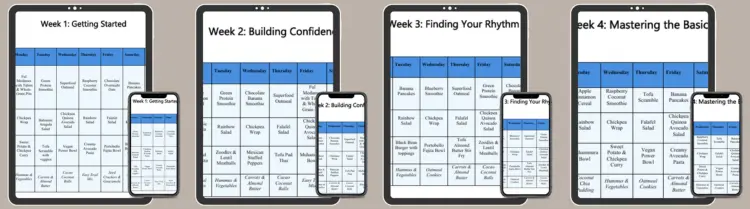
• 4-Week Structured Calendar
• Categorized Weekly Grocery Lists
• Chef-Verified Nutritional Tips
• Family Friendly Meal Prep
• Print & Use Today
How Plant-Based Diets Reverse Insulin Resistance: The Mechanisms
Understanding why a vegan diet for insulin resistance works at the cellular level makes the dietary recommendations logical rather than arbitrary. There are five distinct, well-characterised mechanisms.
Mechanism 1: Soluble Fiber Slows Glucose Entry
Soluble fiber from oats, legumes, and psyllium forms a viscous gel in the small intestine that physically slows the absorption of glucose from carbohydrate foods. This attenuates the post-meal glucose spike and the insulin response required to manage it. Every glucose spike avoided is a reduction in the insulin load on pancreatic beta cells and peripheral insulin receptors. Over weeks and months, reducing peak glucose and insulin exposure measurably improves insulin receptor sensitivity. A vegan diet built on whole plant foods delivers 40-70g fiber daily, approximately 2-3x the fiber intake of the average Western omnivore diet.
Mechanism 2: Resistant Starch Improves Insulin Signalling Via the Gut
Resistant starch, found in cooled cooked potatoes, green bananas, legumes, and cooled rice, passes undigested to the large intestine where it ferments to produce butyrate. Butyrate improves insulin sensitivity through multiple pathways: it activates GPR41 and GPR43 receptors on gut cells that signal to the pancreas, it inhibits histone deacetylase in liver cells (improving hepatic insulin signalling), and it reduces systemic inflammation that drives peripheral insulin resistance. A high-resistant-starch vegan diet is a direct gut-based intervention for the pancreatic signalling pathways that control insulin response.
Mechanism 3: Polyphenols Activate AMPK
AMPK (adenosine monophosphate-activated protein kinase) is the master metabolic switch in cells. When activated, it mimics the metabolic effects of exercise and caloric restriction, improving glucose uptake, reducing hepatic glucose production, and improving insulin sensitivity. Multiple plant polyphenols activate AMPK directly: berberine (from barberries), resveratrol (red grapes, peanuts), quercetin (apples, onions), and EGCG from green tea all show AMPK-activating effects in clinical research reviewed at Examine.com. A polyphenol-rich plant diet is a daily AMPK activation protocol that operates continuously rather than only during exercise.
Mechanism 4: Low Saturated Fat Reduces Intramyocellular Lipid
Intramyocellular lipid (IMCL) is fat accumulated inside muscle cells. High IMCL directly impairs insulin signalling by interfering with the insulin receptor substrate (IRS-1) phosphorylation cascade. High saturated fat diets, particularly palmitic acid from animal products, drive IMCL accumulation. Plant-based diets low in saturated fat reduce IMCL over 8-12 weeks, restoring the intracellular signalling environment that allows insulin receptors to function normally. This is one of the most direct mechanisms by which a vegan diet for insulin resistance works at the muscle cell level independently of changes in body weight.
Mechanism 5: Caloric Efficiency Through Food Volume
High-fiber plant foods deliver satiety at lower caloric density than animal foods and processed foods. A bowl of lentil soup fills the stomach with 300 calories. The equivalent caloric satiety from cheese or meat requires significantly fewer grams but more calories. The result is that plant-based diets naturally create mild caloric restriction without deliberate portion control, driving modest weight loss. Even 5-7% body weight reduction dramatically improves insulin sensitivity because adipose tissue, particularly visceral fat, produces adipokines that drive insulin resistance. The gut health connection to metabolic health is covered in the vegan gut health guide.
The 8 Most Powerful Plant Foods for Insulin Sensitivity
These eight foods stand out in the clinical evidence for their direct and measurable effects on insulin sensitivity, fasting glucose, and HOMA-IR. Each addresses the insulin resistance problem through a distinct mechanism.
1. Lentils
GI: 32 (very low)
The lowest glycaemic legume. High resistant starch plus soluble fiber creates a double glucose-dampening effect. Clinical trials show 35g of lentil consumption daily reduces fasting glucose and improves insulin sensitivity independently of weight change. Also the highest iron legume for plant-based eaters.
2. Oats (Rolled or Steel-Cut)
GI: 55 (medium), but GL: 13 (low)
Beta-glucan, the soluble fiber in oats, forms a highly viscous gel that dramatically slows gastric emptying and glucose absorption. Meta-analyses confirm beta-glucan reduces fasting glucose and post-meal glucose peaks. Steel-cut oats deliver more beta-glucan and have a lower glycaemic response than rolled oats. Avoid instant oat products which have higher GI.
3. Broccoli (Sulforaphane)
Active compound: sulforaphane
Sulforaphane activates Nrf2 signalling and AMPK simultaneously, producing direct insulin-sensitising effects in liver cells. A randomised trial found sulforaphane-rich broccoli sprout extract reduced fasting blood glucose in pre-diabetic obese individuals significantly compared to placebo. Regular broccoli consumption consistently associates with better glycaemic markers in observational data.
4. Berries (All Varieties)
Key compounds: anthocyanins, quercetin, pterostilbene
Berry polyphenols improve insulin signalling through multiple pathways including AMPK activation, alpha-glucosidase inhibition (slowing carbohydrate digestion), and reduction of post-meal oxidative stress. Blueberry polyphenols specifically improve insulin sensitivity in obese insulin-resistant adults in RCTs. Daily berry consumption is one of the highest-evidence dietary interventions for metabolic health in plant-based eating.
5. Cinnamon
Active compound: cinnamaldehyde, proanthocyanidins
Cinnamon improves insulin receptor sensitivity by activating insulin receptor tyrosine kinase, increasing glucose transporter-4 (GLUT-4) activity in muscle cells, and inhibiting protein-tyrosine phosphatase 1B (which normally deactivates the insulin receptor). 1-6g daily in meta-analyses shows consistent fasting glucose and HbA1c improvement. The most evidence-supported culinary spice for glycaemic control.
6. Apple Cider Vinegar
Active compound: acetic acid
Acetic acid inhibits salivary amylase and pancreatic amylase activity, slowing starch digestion. It also activates AMPK in liver cells independently of the amylase pathway. Clinical trials show consuming 2 tablespoons of ACV before a high-carbohydrate meal reduces post-meal glucose by 20-35% in insulin-resistant individuals. The effect is acute and meal-specific rather than cumulative.
7. Green Tea (EGCG)
Active compound: epigallocatechin gallate (EGCG)
EGCG directly activates AMPK, improves GLUT-4 translocation to cell membranes (increasing glucose uptake without insulin), and reduces intestinal glucose absorption. Regular green tea consumption (3-5 cups daily) associates with significantly lower fasting glucose, lower HbA1c, and better HOMA-IR in systematic reviews. The combination of caffeine and EGCG produces additive metabolic effects.
8. Psyllium Husk
Active compound: highly viscous soluble fiber
Psyllium husk forms one of the most viscous gels of any dietary fiber, with a water-holding capacity 100x its own weight. This viscosity effect is unmatched by any whole food fiber. Added to meals or taken before eating, psyllium reduces post-meal glucose peaks by 20-40% in insulin-resistant individuals. It is the single most concentrated fiber intervention available from a plant source.
28-Day Vegan Meal Plan
+ Grocery List
Complete Solution · Nutritionist-Approved · Print & Use Today
Read on any device · No apps needed
Glycaemic Index vs. Glycaemic Load on a Vegan Diet
Glycaemic index (GI) rates how fast a food raises blood glucose. Glycaemic load (GL) accounts for the actual carbohydrate quantity per realistic serving. GL is the more useful clinical metric: a food can have a high GI but a low GL if its realistic serving is small. Watermelon has a high GI (76) but a very low GL (4) because a typical slice contains little carbohydrate.
The chart below compares the GI and GL of common vegan carbohydrate foods. The goal for insulin resistance management is to favour foods in the low-GL zone regardless of their GI.
The practical insight from this chart: lentils, chickpeas, and black beans have the lowest GL of any carbohydrate-containing plant food. Sweet potato has a moderate GL despite its reputation as a high-sugar food. White rice and white bread have very high GL values and should be replaced with legumes, quinoa, or whole grain alternatives as the primary carbohydrate base for people managing insulin resistance. The complete low-glycaemic plant food framework is covered in the low-carb vegan meal plan guide.
Fiber, Resistant Starch, and Vinegar: The Three Dietary Tools
Beyond individual foods, three specific dietary tools have the strongest evidence base for acute and chronic improvement in insulin sensitivity. Each works through a different mechanism and the three are additive when used together.
Tool 1: Soluble Fiber (Target 15-25g Daily)
Soluble fiber is the most extensively studied dietary intervention for insulin resistance. The specific viscous fiber types with the strongest evidence are:
- Beta-glucan from oats: 3g daily (1 serving of oats) reduces post-meal glucose peaks measurably
- Pectin from apples and pears: forms a gel that slows gastric emptying
- Psyllium husk: the most concentrated viscous soluble fiber available as a supplement or food addition
- Inulin from garlic, onion, leek, and asparagus: feeds Bifidobacterium species that produce butyrate for gut-based insulin signalling improvement
The high-fiber plant food guide covers the complete fiber spectrum at the high fiber vegan foods guide.
Tool 2: Resistant Starch (30-40g Daily)
Resistant starch (RS) is starch that resists digestion in the small intestine and reaches the large intestine intact. It is one of the most powerful food-derived interventions for gut-based insulin signalling. Best plant sources by RS type:
- RS2 (raw or minimally processed): green (unripe) bananas, raw oats, raw potato starch. Highest RS content but not always practical.
- RS3 (retrograde starch): cooked and then cooled potatoes, rice, pasta, and legumes. Cooling converts some digestible starch to resistant starch. A potato salad made with cooled cooked potatoes delivers significantly more RS than the same potato eaten hot.
- RS4 (chemically modified): certain processed foods. Lower relevance for whole food plant diets.
Practical daily RS strategy: replace hot white rice with cooled cooked lentils or a cooled grain salad. Eat overnight oats (cooled) rather than hot oatmeal when convenient.
Tool 3: Acetic Acid (Apple Cider Vinegar or Other Vinegars)
Acetic acid works by two mechanisms. First, it inhibits amylase enzymes that digest starches, slowing carbohydrate breakdown and glucose entry into circulation. Second, it activates AMPK in liver and muscle cells directly. The evidence-based protocol:
- 1-2 tablespoons of apple cider vinegar (or any vinegar) in water before or during the highest-carbohydrate meal of the day
- Reduces post-meal glucose by 20-35% in insulin-resistant individuals in controlled trials
- Effect is acute and meal-specific: timing matters. Take it before eating, not hours later.
- Caution: undiluted vinegar damages tooth enamel. Always dilute in at least 200ml of water. Drink through a straw if used daily long-term.
- Contraindicated with certain diuretics and insulin medications: check with a healthcare provider if on medication.
Psst..just to add: reading about anti-inflammatory eating and actually eating that way every day are two very different things. The 28-Day Vegan Meal Plan gives you 40+ recipes, a full shopping list, and a 28-day calendar. No subscription.
Get the Plan →Meal Timing and Insulin: The Intermittent Fasting Connection
When you eat matters as much as what you eat for insulin resistance management. The timing of food intake relative to the circadian rhythm, and the fasting periods between meals, directly affect insulin secretion patterns and receptor sensitivity.
Insulin sensitivity follows a clear circadian pattern: it is highest in the morning, moderate at midday, and lowest in the evening and at night. The same meal eaten at 8am produces a significantly smaller insulin response than the same meal eaten at 8pm. This means the timing of carbohydrate consumption across the day is a metabolic tool with measurable effects on HOMA-IR.
Eat Your Most Complex Carbs Here
- Highest insulin sensitivity of the day
- Steel-cut oats, lentil dishes, legume-based breakfast
- Front-loading calories and carbohydrates improves HOMA-IR vs back-loading
- Skipping breakfast worsens glucose control throughout the day
Main Meal with Protein + Fiber First
- Eat protein and fiber components before carbohydrate components
- This food order strategy reduces post-meal glucose by 30-40% in studies
- Legume-based main dishes with vegetables
- Insulin sensitivity is still adequate but declining from morning peak
Low-GL Snacks Only
- If a snack is needed: nuts, seeds, or raw vegetables with hummus
- Avoid high-carbohydrate afternoon snacks: biscuits, fruit juice, refined crackers
- Green tea or cinnamon tea here activates EGCG and cinnamaldehyde pathways
Reduce Carbohydrate Load
- Insulin sensitivity is lowest in the evening
- Focus on protein and non-starchy vegetables
- Reduce grain and root vegetable portions compared to morning meals
- Apple cider vinegar before this meal is highest value here
Close the Eating Window
- Late eating dramatically impairs insulin sensitivity due to circadian misalignment
- The pancreas produces less insulin at night for the same glucose load
- A 12-14 hour overnight fast from last meal to breakfast creates the natural insulin-sensitising effect of intermittent fasting
12-16 Hours: The IF Connection
- A 12-14 hour overnight fast (10pm to 10am) is the minimum beneficial IF window
- Extends to 16:8 if weight loss alongside metabolic improvement is the target
- Full vegan intermittent fasting framework: IF guide
The 7-Step Daily Vegan Insulin Resistance Protocol
This protocol consolidates all the mechanisms, foods, and timing strategies into a daily system. Each step addresses a different element of insulin resistance pathology. Applied consistently for 12-16 weeks, measurable improvements in fasting glucose, HbA1c, and HOMA-IR are expected in the majority of people with stages 2-3 insulin resistance.
Morning Anchor: Steel-Cut Oats with Berries and Cinnamon
Beta-glucan from oats, anthocyanins from berries, and cinnamaldehyde from cinnamon deliver three distinct glucose-lowering mechanisms in one breakfast. This is the most evidence-concentrated single meal available for insulin resistance.
- Steel-cut oats (not rolled, not instant): maximum beta-glucan content
- Half a cup of blueberries or mixed berries: AMPK activation and alpha-glucosidase inhibition
- 1 teaspoon cinnamon: insulin receptor sensitisation
- 1 tablespoon ground flaxseed: omega-3 ALA and additional viscous fiber
Pre-Meal Vinegar at the Highest-Carbohydrate Meal
1-2 tablespoons apple cider vinegar in 200ml water consumed 10-15 minutes before the largest carbohydrate meal of the day. This is the single highest-impact acute intervention for post-meal glucose control.
Replace All White Grains with Legumes or Whole Grains
White rice, white bread, and white pasta are the single largest avoidable contributors to glycaemic load in most diets. The replacement targets:
- White rice: replace with lentils, chickpeas, or cooled cooked brown rice
- White bread: replace with whole grain sourdough or legume-based wraps
- White pasta: replace with lentil pasta or use significantly smaller portions of whole grain pasta
Daily Legume Serving (Minimum 1 Cup Cooked)
Legumes are the cornerstone food of a vegan diet for insulin resistance. Low GI, high resistant starch, high soluble fiber, high protein for satiety, high magnesium for insulin receptor function. A daily cup of lentils, black beans, chickpeas, or edamame addresses the insulin resistance problem through every mechanism simultaneously.
- Soak dried legumes overnight: improves nutrient availability and reduces gas
- Cooled cooked legumes have higher resistant starch than freshly cooked
- Rotate legume varieties for microbiome diversity
Green Tea: 3-5 Cups Daily
3-5 cups of green tea daily delivers clinically meaningful EGCG doses that activate AMPK, improve GLUT-4 translocation, and reduce intestinal glucose absorption. Green tea is the most evidence-supported beverage for insulin sensitivity improvement. Replace coffee after noon with green tea to combine caffeine reduction (which improves overnight insulin sensitivity) with EGCG delivery.
Eat in Food Order: Fiber and Protein Before Carbohydrate
Research published and reviewed at PubMed confirms that eating vegetables and protein before the carbohydrate component of the same meal reduces post-meal glucose by 30-40%. The practical rule: eat the salad or vegetables first, then the protein (tofu, lentils), then the grain component. This food sequencing strategy has no cost, no preparation change, and produces immediate results at every meal.
Close the Eating Window: 12-14 Hour Overnight Fast Minimum
Finish eating by 7-8pm and do not eat again until 7-9am. This 12-13 hour fasting window allows insulin levels to fall completely overnight, restoring receptor sensitivity before the next day's eating. This is the minimum intermittent fasting protocol for insulin resistance benefit. The full IF framework for plant-based eating is at the vegan intermittent fasting guide.
For people managing insulin resistance alongside weight plateau challenges, the vegan weight loss plateau guide covers the intersection of metabolic resistance and plant-based fat loss in detail.
Chef Section: MENA Low-Glycaemic Traditional Cooking
Twenty years of professional MENA and Mediterranean kitchen experience reveals a culinary tradition that was low-glycaemic before that term existed. Traditional MENA cooking is built around legumes, slow-cooked whole grains, spice-driven flavour, and olive oil, the precise dietary architecture that a vegan diet for insulin resistance requires. The original MENA diet before the urbanisation of food culture was naturally optimal for metabolic health.
Four MENA Low-Glycaemic Cooking Principles
1. The Legume-First Plate
Traditional MENA meals are structured around a legume base rather than a grain base. Ful medames (fava beans), hummus (chickpeas), mujaddara (lentils with caramelised onion), and fasolia (bean stew) are the protein and carbohydrate anchors of everyday eating. The GI and GL of these dishes is exceptional by any comparison. Ful medames has a GL of approximately 5-7 per serving. Mujaddara has a GL of 8-10. A traditional MENA lunch structured around any of these dishes is profoundly lower in glycaemic impact than the Western lunch pattern built around bread, white rice, or pasta.
2. Slow Cooking as Resistant Starch Optimisation
The traditional MENA technique of long, slow cooking in clay pots and then allowing dishes to cool before serving is an inadvertent resistant starch optimisation. Slow-cooked then cooled legumes convert a higher proportion of their starch to the resistant form than rapidly boiled and immediately served legumes. The traditional practice of eating legume dishes the next day as leftovers, which is standard across MENA domestic cooking, delivers higher resistant starch content than the freshly cooked version. Nutritional science has now validated this practice. The MENA kitchen was optimising resistant starch before the term was coined.
3. Spice as Metabolic Medicine: Cumin, Turmeric, Fenugreek
Three MENA spices used daily in traditional cooking have direct evidence for insulin sensitisation:
- Fenugreek (helba): contains 4-hydroxyisoleucine, an amino acid that directly stimulates insulin secretion. Also rich in galactomannan soluble fiber that slows glucose absorption. Used in MENA bread, spice blends, and legume dishes.
- Cumin: improves insulin sensitivity through antioxidant mechanisms. Reduces glycation end-products. Used generously in lentil soup, ful medames, and grain dishes throughout MENA cooking.
- Turmeric: curcumin activates AMPK and reduces NF-kB inflammatory signalling that drives insulin resistance. Daily use in rice, lentil, and vegetable dishes throughout MENA cooking.
4. Olive Oil as the Default Fat: Oleocanthal and Oleic Acid
MENA cooking uses extra virgin olive oil as the primary fat in a way no other culinary tradition does. The oleic acid in olive oil does not drive intramyocellular lipid accumulation the way saturated fat does, preserving insulin receptor function at the muscle cell level. Oleocanthal, olive oil's primary polyphenol, inhibits the same inflammatory enzymes as ibuprofen and reduces the low-grade inflammation that drives insulin resistance. A diet that uses generous extra virgin olive oil daily, as traditional MENA cooking does, is fundamentally anti-inflammatory and insulin-sensitising at the lipid level.
The MENA Insulin Resistance Day: A Professional Kitchen Template
- Breakfast: ful medames with olive oil, cumin, and lemon + 1 tsp cinnamon in warm herbal tea (GL approximately 6)
- Lunch: mujaddara (cooled lentil and rice dish) with roasted broccoli and tahini + green salad eaten first (GL approximately 12)
- Afternoon: 2 cups green tea + small handful walnuts
- Dinner: slow-cooked chickpea stew with turmeric and fenugreek + minimal grain component (GL approximately 8)
- Pre-largest meal: 1 tablespoon apple cider vinegar in water
- Eating window closed by 7:30pm. 13-hour overnight fast.
For the complete MENA recipe library that builds this framework into practical daily cooking, the Middle Eastern vegan recipes guide covers the full range of dishes.
Putting It Together: Vegan Diet for Insulin Resistance as a Clinical-Grade Intervention
A vegan diet for insulin resistance is not a complementary addition to insulin resistance management. In stages 2 and 3 of the metabolic continuum (compensated resistance and pre-diabetes), it is a primary intervention with clinical trial evidence for effectiveness equivalent to or exceeding first-line pharmaceutical approaches in motivated individuals. The mechanisms are multiple, the evidence is consistent, and the dietary changes required are achievable without specialist resources.
The five mechanisms of action (soluble fiber, resistant starch, polyphenol AMPK activation, reduced saturated fat, and caloric efficiency) all operate simultaneously in a well-planned plant-based diet. The three tools (fiber, resistant starch, vinegar) can be deployed within days. The food order strategy (fiber before protein before carbohydrate) costs nothing and produces immediate results. The 12-14 hour overnight fast requires no supplementation or caloric restriction, only earlier dinner timing.
A vegan diet for insulin resistance built on legumes, berries, oats, green tea, and the MENA culinary tradition of low-glycaemic whole food cooking is one of the most evidence-supported and practically achievable therapeutic dietary strategies available for reversing pre-diabetes and metabolic syndrome before they progress to conditions requiring pharmaceutical management.

28-Day Vegan Meal Plan + Grocery list.
Transform your lifestyle with our comprehensive guide. This isn't just a recipe book; it's a complete system designed for success:
- The Vegan Guide: Essential transition tips and nutritional benefits.
- 40+ Chef Recipes: Breakfast, lunch, and dinner with high-quality photos.
- 4-Week Meal Plan: A fully structured day-by-day calendar.
- Grocery Lists: Categorized weekly lists to save you time and money.
- Photos: High-Quality Recipe Photos.
- Nutritions: Vegan Nutrition Guide Toolkit.
FAQ: 12 Questions About the Vegan Diet for Insulin Resistance
Yes, with significant clinical evidence. Randomised controlled trials of plant-based dietary interventions in insulin-resistant and pre-diabetic populations consistently show improvement in fasting glucose (5-15% reduction), HbA1c (0.4-1.2% reduction), and HOMA-IR (20-30% improvement) within 12-16 weeks. The evidence base is sufficient for major diabetes organisations to recommend plant-based dietary patterns as an evidence-based option for pre-diabetes management. Full reversal, meaning return to stage 1 insulin sensitivity from stages 2-3, is achievable for many people through dietary intervention alone, particularly when combined with modest weight loss and improved physical activity.
Not categorically. The type, fiber content, and glycaemic load of carbohydrates determines their effect on insulin sensitivity. Carbohydrates from lentils (GL 5-7), oats (GL 13), and sweet potato (GL 17) produce very different insulin responses from white rice (GL 29) and white bread (GL 20). The practical rule: replace high-GL refined carbohydrates with low-GL legume-based and whole grain alternatives. Plant-based diets are inherently higher in carbohydrates than omnivore diets, but the clinical evidence shows this is not a problem when the carbohydrates come from legumes, vegetables, and whole grains rather than refined grains and added sugars.
HOMA-IR (Homeostatic Model Assessment of Insulin Resistance) is a calculated index using fasting glucose and fasting insulin levels: HOMA-IR = (fasting glucose × fasting insulin) / 22.5. Values below 1.0 are considered insulin sensitive. Values above 2.0 indicate insulin resistance. Values above 2.5 indicate significant insulin resistance. Plant-based dietary interventions that reduce both fasting glucose and fasting insulin produce proportionally larger reductions in HOMA-IR than interventions that affect only one of the two variables. A vegan diet that reduces fasting insulin by 15% and fasting glucose by 10% can produce a HOMA-IR reduction of 22-25% from the combined effect.
Intermittent fasting improves insulin resistance through two primary mechanisms. First, fasting periods allow insulin levels to fall completely, giving insulin receptors time to upregulate sensitivity without constant insulin stimulation. Second, extended fasting activates autophagy and AMPK, which improve cellular insulin signalling machinery independently of dietary composition. On a vegan diet, the 16:8 intermittent fasting protocol (16 hours fasting, 8-hour eating window) produces additive improvements in insulin sensitivity beyond what the plant-based dietary composition achieves alone. The key practical detail: the eating window should be earlier in the day (7am-3pm or 8am-4pm) rather than later, as morning eating aligns with the circadian peak of insulin sensitivity.
Yes. Soy foods have a very low glycaemic load and contain isoflavones that directly improve insulin sensitivity through oestrogen receptor-beta signalling in pancreatic beta cells. Studies consistently show that soy consumption in insulin-resistant individuals improves fasting glucose and insulin sensitivity. Tofu (GI approximately 18), edamame (GI approximately 18), and tempeh (GI approximately 15) are among the safest carbohydrate-containing plant foods for insulin resistance management. The concern about soy and hormonal effects is not supported by clinical evidence at normal dietary intakes and is covered in detail in the vegan PCOS guide.
The evidence-optimal vegan breakfast for insulin resistance:
- Base: steel-cut oats (not instant) for maximum beta-glucan content
- Berries: half a cup of blueberries or mixed berries for AMPK activation
- Cinnamon: 1 teaspoon for insulin receptor sensitisation
- Seeds: 1 tablespoon ground flaxseed for additional soluble fiber and omega-3
- Protein: hemp seeds or a small portion of nut butter for satiety and leucine
Alternative: a legume-based breakfast such as ful medames with olive oil and cumin, which has an even lower GL than oats. The MENA tradition of legume-first breakfast is metabolically superior to grain-first for insulin resistance.
Yes, substantially. Meta-analyses of fiber supplementation and dietary fiber increase trials show consistent improvements in fasting glucose (mean reduction 0.28 mmol/L), HbA1c (mean reduction 0.55%), and HOMA-IR in type 2 diabetes and pre-diabetes populations. The effect size is largest for viscous soluble fibers (psyllium, beta-glucan, pectin) rather than insoluble fiber. A plant-based diet delivering 40-70g total fiber daily, including 15-25g soluble fiber from oats, legumes, and vegetables, produces fiber-driven glucose improvements that operate independently of caloric restriction or weight change. Fiber is not a secondary benefit of a plant diet for insulin resistance. It is a primary mechanism.
Insulin resistance is present in 65-70% of women with PCOS regardless of body weight. Elevated insulin drives excessive androgen production by the ovarian theca cells, creating many of the hormonal symptoms of PCOS including irregular periods, acne, and hirsutism. A vegan diet for insulin resistance is therefore simultaneously a PCOS management strategy. The plant-based dietary improvements in insulin sensitivity (through fiber, legumes, and low-GL carbohydrates) directly reduce ovarian androgen production and improve PCOS symptom scores in clinical evidence. The PCOS-specific plant diet guide is at the vegan PCOS guide.
Glycaemic index measures how fast a food raises blood glucose relative to pure glucose. Glycaemic load combines GI with the actual carbohydrate content of a realistic serving. GL = (GI x grams of carbohydrate per serving) / 100. The practical difference: watermelon has a high GI (76) but an extremely low GL (4) because a typical slice contains only 6g of carbohydrate. Dates have a moderate GI (42) but a high GL because a typical portion contains a large amount of carbohydrate. For insulin resistance management, GL is the metric that matters because it reflects the actual glucose and insulin demand placed on the body by the food as eaten, not the theoretical speed of a 50g carbohydrate load that nobody actually consumes.
Yes, and the combination is substantially more effective than either alone. Exercise improves insulin sensitivity through AMPK activation (same pathway as plant polyphenols) and by increasing GLUT-4 transporter density in muscle cell membranes, allowing glucose to enter cells without insulin. Diet and exercise activate overlapping and additive pathways. The combination of a low-GL plant-based diet with resistance training (which builds metabolically active muscle tissue) and moderate aerobic exercise (which increases GLUT-4 density acutely) produces the fastest and most durable insulin sensitivity improvements available without pharmaceutical intervention. The metabolism-focused guide is at the vegan metabolism guide.
Low-carb approaches improve insulin resistance primarily by reducing the total glucose and insulin load on the system. However, the evidence for high-fiber plant-based diets is equally strong through different mechanisms, without the nutritional trade-offs of eliminating legumes and whole grains. The most evidence-supported position is: reduce high-GL refined carbohydrates aggressively, but do not reduce low-GL legumes, whole grains, and high-fiber plant foods which improve insulin sensitivity rather than worsening it. A low-GL vegan diet is not the same as a low-carbohydrate diet. The low-carb plant-based framework is explored at the low-carb vegan meal plan guide.
Improvements occur at multiple timescales:
- Acute (same day): apple cider vinegar before meals reduces post-meal glucose within the first use. Food order strategy (fiber before protein before carbs) reduces post-meal glucose by 30-40% immediately.
- Short-term (2-4 weeks): fasting insulin begins to fall as insulin receptor sensitivity improves from reduced saturated fat intake and increased fiber. Weight loss begins if there is a caloric deficit.
- Medium-term (8-12 weeks): measurable fasting glucose reduction, HbA1c begins to fall, HOMA-IR improvement becomes detectable. Most clinical trial endpoints are measured at 12-16 weeks.
- Long-term (6-12 months): sustained insulin sensitivity improvement, potential reversal from pre-diabetes to normal glucose tolerance in motivated individuals with consistent protocol adherence.

Still spending hours figuring out what to eat?
What's included in your download
- 40+ nutritionist-approved recipes
- Complete 28-day calendar
- Meets protein, iron & B12 needs
- Family & meal prep friendly
- Vibrant photo for every recipe
- Simple, common ingredients
Instant PDF download. No subscriptions. No waiting.