Disclaimer: This article is for informational and educational purposes only. It does not constitute medical or nutritional advice. Consult a qualified healthcare professional or registered dietitian for personalised guidance, particularly during pregnancy or if you have a condition affecting fat or nutrient absorption.
Vegan Vitamin A Foods: The Complete Guide to Plant-Based Vitamin A Sources
Preformed vs. Provitamin A: The Essential Distinction
Vitamin A exists in two fundamentally different dietary forms, and understanding the distinction between them is the entire foundation of a vegan vitamin A foods strategy. Getting this wrong leads either to unnecessary anxiety about deficiency or to a false sense of security that colourful vegetables automatically provide adequate vitamin A regardless of how they are prepared and eaten.
Preformed vitamin A (retinol) is the biologically active form found exclusively in animal products: liver, egg yolks, full-fat dairy, and oily fish. It is immediately usable by the body without conversion. A single serving of beef liver can provide 5,000 to 10,000 micrograms of retinol, over a week’s worth of requirement in one sitting. Vegans consume zero preformed vitamin A.
Provitamin A carotenoids are plant-derived pigments that the body can convert to retinol as needed. Beta-carotene is the most abundant and most efficiently converted. Alpha-carotene and beta-cryptoxanthin are also converted but at lower efficiency. These are what vegan vitamin A foods actually provide. The conversion happens primarily in the intestinal wall and liver, regulated by the body’s current retinol status: when body stores are adequate, conversion rate slows. This self-regulation provides a safety mechanism against vitamin A toxicity from plant sources that does not exist with preformed retinol supplements.
The practical implication of the 12:1 conversion ratio is significant. To obtain 900 mcg of retinol activity equivalents (RAE) from beta-carotene alone, a vegan needs to consume 10,800 mcg (10.8mg) of beta-carotene daily from food. One medium sweet potato provides approximately 9,400 mcg. One large carrot provides approximately 8,300 mcg. These foods make the target achievable, but only when eaten consistently, with fat present, and when cooked appropriately to break down the chromoplast matrix that otherwise limits carotenoid release. These conditions are not always met in practice, which is why vegan vitamin A foods require more deliberate attention than plant-based nutrition guides typically acknowledge.

-
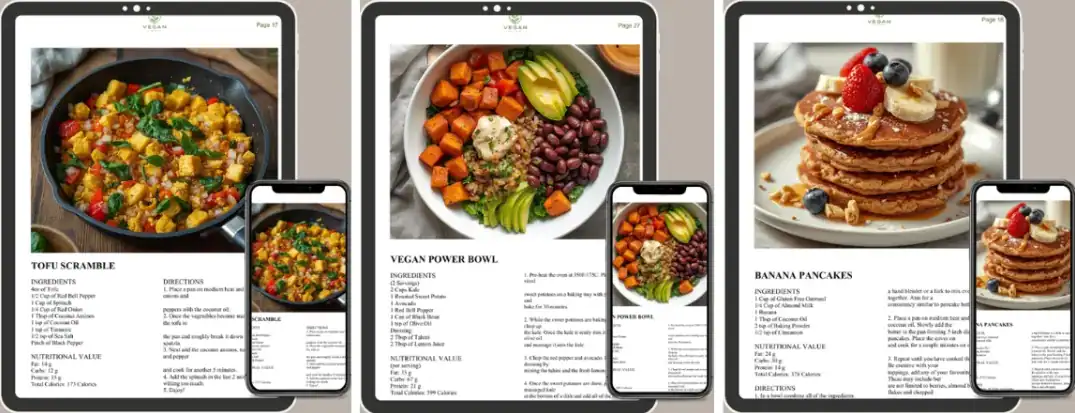
Complete 28-day calendarEvery breakfast, lunch, dinner & snack planned
-
40+ nutritionist-approved recipesVibrant photo for every single dish
-
Easy weekly grocery listsShop smart, spend less, waste nothing
-
Protein, iron & B12 at every mealNutritionally complete — no guesswork
-
Saves 7+ hours weeklyPrint it once, follow it all month
-
Bonus: Nutrition Guide ToolkitVegan tips, guides & family meal prep
The Beta-Carotene Conversion Problem: What Most Guides Miss
The conversion of beta-carotene to retinol is not a fixed, reliable process. It is highly variable across individuals and significantly affected by multiple dietary and physiological factors. This variability is the most under-discussed aspect of vegan vitamin A nutrition, and it explains why some vegans eating plenty of orange and green vegetables can still have suboptimal vitamin A status.
The BCMO1 genetic variant finding is the most significant. A 2009 study and subsequent research have identified common single-nucleotide polymorphisms (SNPs) in the BCMO1 gene that reduce conversion efficiency by 32 to 69% compared to normal converters. Approximately 45% of people carry at least one of these variants. Crucially, there is no consumer genetic test that reliably identifies who carries these variants without specific research-grade sequencing. This means nearly half the vegan population may be significantly less efficient at converting beta-carotene than current dietary recommendations assume, and they would have no way of knowing it from routine nutrition guidance.
Who Is Most at Risk of Inadequate Vegan Vitamin A Status
- Pregnant vegans: Vitamin A requirement increases to 770 mcg RAE, fetal development is acutely sensitive to both deficiency and excess
- Vegans with thyroid conditions: Hypothyroidism reduces BCMO1 activity. The vegan thyroid guide covers this intersection
- People following very low-fat WFPB diets: Fat is non-negotiable for carotenoid absorption
- Vegans with gut health issues: IBD, celiac disease, or significant dysbiosis reduces intestinal conversion capacity
- Anyone eating predominantly raw vegetables: Beta-carotene bioavailability from raw plant foods is 3 to 6 times lower than from cooked
The zinc connection is worth noting specifically because zinc deficiency is common in plant-based diets due to phytate binding. Zinc is required not just for immune function and wound healing but for the synthesis of retinol-binding protein, which transports vitamin A from the liver to tissues. A vegan with suboptimal zinc status may have adequate liver retinol stores but impaired delivery to peripheral tissues. This creates functional vitamin A insufficiency even when serum retinol appears borderline adequate. Ensuring zinc sufficiency from pumpkin seeds, hemp seeds, and legumes as covered in the vegan zinc guide is therefore directly relevant to vitamin A status.
Top Vegan Vitamin A Foods Ranked
The following ranking uses retinol activity equivalents (RAE) per 100g of food cooked, which accounts for the 12:1 beta-carotene to retinol conversion ratio. Raw values would be 3 to 6 times lower due to reduced bioavailability. All values are approximate from USDA FoodData Central. Eating these vegan vitamin A foods cooked and with a source of fat is essential for meaningful absorption.
Sweet potato and carrot dominate the vegan vitamin A foods list by a significant margin. A single medium baked sweet potato with skin (approximately 130g) provides close to the full adult daily requirement for vitamin A in RAE terms, assuming normal BCMO1 conversion and adequate dietary fat at the same meal. This is one of the most striking nutrient density figures in plant-based nutrition: one common, inexpensive vegetable covering an entire day’s vitamin A need in one serving.
The dark leafy green contribution is important and often underappreciated. Kale and spinach contain beta-carotene alongside lutein and zeaxanthin, carotenoids that accumulate specifically in the retina and are the nutritional foundation of macular health. These vegetables do double duty: supporting both systemic vitamin A status and the specific carotenoid protection that eyes need independently of retinol. The broader antioxidant function of leafy greens is covered in the vegan vitamin E guide, where the synergy between carotenoids and tocopherols for oxidative protection is discussed.

Spotlight: 6 Key Plant-Based Vitamin A Foods
The single most powerful vegan vitamin A food. Bake with skin on for maximum nutrient retention. Eat with olive oil or nut butter for fat-mediated absorption. Also provides potassium, vitamin C, and manganese.
Boiling or steaming ruptures cell walls and significantly increases beta-carotene release compared to raw. Roasting with olive oil is the single best preparation for maximum vegan vitamin A absorption from carrots.
High beta-carotene plus lutein and zeaxanthin specifically concentrated in retinal tissue. Lightly steam or saute in olive oil. Also provides vitamin K, vitamin C, calcium, and iron, making it the most nutritionally comprehensive vegan vitamin A food.
Roasted butternut squash provides over half the daily vitamin A requirement per 100g cooked serving, alongside vitamin C and potassium. The carotenoids are concentrated in the bright orange flesh and roasting with fat is optimal.
Cooking spinach reduces oxalate content and concentrates beta-carotene significantly. A half-cup of cooked spinach provides more beta-carotene than several cups of raw. Pairs naturally with olive oil or tahini for fat-mediated absorption.
Provides beta-carotene alongside the highest vitamin C content of any common vegetable. Vitamin C and vitamin A work synergistically for immune function and skin health. Eat raw with hummus (fat present) or roasted with olive oil for dual nutrient benefit.
What Vitamin A Actually Does: The Four Critical Functions
Vitamin A is not a single-function micronutrient. Its biological roles span vision, immune defence, epithelial cell maintenance, and embryonic development. Understanding all four functions helps explain why subclinical insufficiency has wide-ranging effects that are easy to misattribute to other causes on a vegan diet.
The Four Biological Roles of Vitamin A
Vision: Retinal (oxidised retinol) combines with opsin proteins to form rhodopsin in rod photoreceptor cells, the primary pigment for dim-light and night vision. The earliest clinical sign of vitamin A deficiency is night blindness. Lutein and zeaxanthin from the same orange and green vegetables protect the retina from oxidative damage independently of this rhodopsin pathway.
Immune function: Vitamin A regulates the differentiation of T helper cells, maintains the integrity of mucosal barriers (gut, respiratory, urogenital), and supports the production of secretory IgA antibodies at mucosal surfaces. Vitamin A deficiency increases susceptibility to infections, particularly respiratory and gastrointestinal. For vegans concerned about immune resilience, vitamin A status alongside vitamin C and vitamin D forms the core immune nutrition triad.
Epithelial and skin cell maintenance: Retinoic acid (the gene-regulatory form of vitamin A) controls the differentiation and proliferation of epithelial cells throughout the body, including skin, the gut lining, the cornea, and respiratory mucosa. Inadequate vitamin A produces keratinisation, the abnormal accumulation of keratin protein in epithelial cells, leading to rough, dry skin, impaired gut barrier function, and dry eyes.
Embryonic development: Retinoic acid is a master regulator of embryogenesis, directing the development of the heart, limbs, eyes, and nervous system. Both deficiency and excess are teratogenic. Pregnant vegans must ensure adequate beta-carotene intake from vegan vitamin A foods while avoiding high-dose preformed vitamin A supplements.
The immune-barrier connection is particularly relevant for vegans managing gut health. Vitamin A maintains the tight junctions between intestinal epithelial cells that prevent bacterial antigens from entering systemic circulation. When vitamin A is insufficient, gut barrier integrity weakens, potentially worsening the intestinal permeability that underlies many inflammatory and autoimmune conditions. A well-functioning gut lining is critical for both carotenoid absorption and systemic immune defence.
Maximising Absorption: The Fat Connection and Food Preparation
Beta-carotene is a fat-soluble pigment. Like all fat-soluble compounds, it dissolves in fat and is absorbed through the same intestinal pathways as dietary lipids. Without fat present at the same meal, the majority of beta-carotene from vegan vitamin A foods passes through the gut unabsorbed. This is not a minor adjustment: studies show that eating carotenoid-rich vegetables with zero added fat reduces absorption by 85 to 95% compared to eating them with 3 to 5g of fat.
The Preparation Hierarchy for Maximum Vegan Vitamin A Absorption
Best: Roasted in olive oil. Heat ruptures chromoplasts, fat facilitates micelle formation in the gut, absorption is maximised. Roasted carrots in olive oil deliver 3 to 6 times more absorbable beta-carotene than raw carrots with no fat.
Good: Steamed or boiled, then dressed with olive oil, tahini, or avocado. Cooking alone improves bioavailability significantly. Adding fat at the table maintains the benefit without cooking in oil.
Moderate: Raw with fat. A carrot dipped in hummus still absorbs more beta-carotene than a plain raw carrot, but less than a cooked carrot with fat. Raw is acceptable when fat is present, not without it.
Poor: Raw with no fat. Plain raw vegetable sticks with no dip. Green smoothies without nut butter, avocado, or seeds. Beta-carotene absorption in this context is minimal regardless of the quantity of vegan vitamin A foods consumed.
Food particle size also matters. Chopped, grated, or blended vegetables release more beta-carotene than whole vegetables of the same weight, because mechanical disruption of plant cell walls pre-releases the carotenoid from its chromoplast matrix before digestion begins. This is why blended soups and pureed squash deliver more available beta-carotene than equivalent whole pieces of the same vegetable. For practical vegan vitamin A foods optimisation: cook orange and green vegetables, add fat to every serving, and use chopped or blended preparations regularly.
7-Step Vegan Vitamin A Protocol
Eat sweet potato, carrot, or butternut squash at least four times per week, cooked. These three vegetables are the most reliable and concentrated vegan vitamin A foods available. A single medium baked sweet potato or a serving of roasted carrots covers most or all of the adult daily vitamin A requirement assuming normal conversion. Four servings per week provides consistent beta-carotene loading that keeps liver retinol stores replenished even at typical conversion rates.
Always eat vegan vitamin A foods with a fat source. This is the single most impactful practical step in this protocol. Olive oil, avocado, tahini, nut butter, or a handful of seeds with every orange and green vegetable serving. Never eat plain raw carrot sticks, plain dressed salads, or fat-free vegetable dishes and expect meaningful vitamin A absorption. The fat rule applies to every meal containing beta-carotene rich food.
Cook orange and green vegetables rather than eating them exclusively raw. Raw vegetables are valuable for enzymes, vitamin C, and probiotics but are significantly inferior for beta-carotene absorption. Roasting, steaming, and boiling all substantially increase bioavailable vitamin A from plant foods. Balance raw vegetable intake with cooked preparations throughout the week. Raw spinach in a smoothie contributes very little vitamin A; sauteed spinach in olive oil contributes substantially.
Include dark leafy greens daily for beta-carotene plus lutein and zeaxanthin. Kale, spinach, collard greens, and Swiss chard provide beta-carotene alongside eye-specific carotenoids. The lutein and zeaxanthin in these greens are not converted to vitamin A but are essential for retinal health independently of retinol. Eating leafy greens daily delivers the full carotenoid spectrum that eyes need. Pair with olive oil or tahini at every serving. The broader case for dark leafy greens in a plant-based diet is made in the vitamin K guide, where these same vegetables also top the K1 rankings.
Ensure adequate zinc status for retinol transport. Zinc is required for retinol-binding protein synthesis, which delivers vitamin A from the liver to tissues. Zinc deficiency creates functional vitamin A insufficiency even when dietary intake and liver stores are adequate. Eat pumpkin seeds, hemp seeds, lentils, and cashews daily. Soak legumes and seeds to reduce phytate binding. If you do not regularly eat these foods, consider a zinc supplement at 8 to 11mg per day to close the gap that plant diets commonly produce.
Monitor vitamin A status if you fall into a higher-risk group. Pregnant vegans, those with thyroid conditions, those following very low-fat diets, and those with gut absorption issues should discuss serum retinol testing with a healthcare provider. Serum retinol below 0.70 micromol/L indicates deficiency. Levels between 0.70 and 1.05 micromol/L suggest marginal status. If testing shows concern, a small dose of preformed vegan vitamin A from lichen-derived supplements (note: these exist but are rarer than plant beta-carotene supplements) or algae-source retinol should be discussed with a dietitian. The vegan blood test guide covers which markers to request and how to interpret results.
Do not supplement with high-dose isolated beta-carotene if you smoke. This warning applies to all dietary approaches. Two large trials (ATBC and CARET) found that high-dose isolated beta-carotene supplementation significantly increased lung cancer risk in smokers. Dietary beta-carotene from whole vegan vitamin A foods does not carry this risk. If you smoke and are considering beta-carotene supplements, do not. Focus entirely on food sources.
Chef’s Perspective: MENA Orange and Green Traditions as Vitamin A Foundations
In over twenty years of professional cooking across Lebanon, the Gulf, and Saudi Arabia, I have worked with vegetables that are now understood to be among the richest vegan vitamin A foods available, prepared in ways that maximise exactly what we now know matters most for carotenoid absorption: cooking in oil, using bold spices, and building meals around these orange and green ingredients rather than treating them as garnishes.
The MENA tradition of slow-cooking pumpkin and squash in olive oil with onion, cumin, and coriander is a perfect vitamin A absorption protocol dressed as regional comfort food. The heat breaks down the pumpkin’s cell walls, the olive oil creates the fat matrix needed for micelle formation in the gut, and the bright orange colour signals the beta-carotene density that your body will convert to retinol. A Lebanese mahshi, stuffed courgette or pumpkin cooked in tomato and olive oil, delivers meaningful vitamin A in a format that has been nutritionally optimised by centuries of practical cooking wisdom.
Carrots appear throughout MENA cooking in ways that Western salad bars do not match. Moroccan carrot salads cooked in olive oil with cumin and preserved lemon, Saudi side dishes of spiced roasted root vegetables, Lebanese carrot soups enriched with olive oil and finished with lemon: every one of these preparations cooks the carrot (releasing beta-carotene from chromoplasts), adds fat (enabling absorption), and uses acidic finishing agents that help preserve the carotenoid content. The methodology is complete.
Dark leafy greens in the form of mloukhieh (jute leaves), molokhia cooked in olive oil, and the generous use of parsley across MENA cooking add the lutein and zeaxanthin layer that sweet potato and carrot do not provide. A meal including both an orange vegetable and a dark leafy green cooked in olive oil covers the full spectrum of plant-based vitamin A nutrition. This is what a well-constructed MENA plant-based plate does naturally, without any nutritional planning beyond following the culinary tradition.
Frequently Asked Questions About Vegan Vitamin A Foods
Can vegans get enough vitamin A from plant foods?
Yes, for most vegans eating varied diets with regular orange and green vegetables cooked with fat. Sweet potato, carrot, kale, spinach, and butternut squash provide substantial beta-carotene that the body converts to retinol. However, the conversion is less efficient than commonly presented in basic nutrition guides, and several factors including genetics, thyroid function, fat intake, and cooking method significantly affect how much retinol is actually produced. Vegans eating these foods consistently, cooked, and with dietary fat present can meet their vitamin A requirements. Those in higher-risk groups should monitor their status.
What is the difference between retinol and beta-carotene?
Retinol is preformed vitamin A, the biologically active form found only in animal products. It is immediately usable by the body. Beta-carotene is a provitamin A carotenoid found in plants that the body must convert to retinol before use. The conversion requires the BCMO1 enzyme, dietary fat for absorption, and adequate thyroid function. The official conversion ratio is 12:1 (12 mcg beta-carotene yields 1 mcg retinol activity equivalent), but real-world conversion in many individuals is closer to 20:1 or higher. Beta-carotene cannot cause vitamin A toxicity because conversion is regulated by body stores. Preformed retinol at high supplemental doses can cause toxicity.
Why do vegans need to cook their vitamin A-rich vegetables?
Beta-carotene is trapped inside chromoplasts, specialised plant cell organelles. These act as a protective barrier that limits carotenoid release during digestion when vegetables are raw. Cooking, whether steaming, boiling, or roasting, ruptures chromoplast membranes and releases beta-carotene into the food matrix where digestive processes can access it. Studies consistently show 3 to 6 times greater beta-carotene bioavailability from cooked vegetables compared to raw equivalents. This does not mean all vegetables should be cooked, but specifically for maximising vitamin A from vegan vitamin A foods, cooking is significantly more effective than eating raw.
Is sweet potato really the best vegan vitamin A food?
In practical daily eating terms, yes. Sweet potato provides approximately 961 mcg RAE per 100g cooked, covering more than the full adult daily vitamin A requirement in a single serving of a common, inexpensive, widely available food. It is also rich in potassium, vitamin C, manganese, and fibre. The combination of exceptional vitamin A provision with a broad overall nutritional profile makes baked sweet potato with olive oil or nut butter the single most practical vegan vitamin A foods strategy available. Carrot runs a close second and is arguably more versatile across different meal types.
Can I overdose on vitamin A from plant foods?
No. You cannot develop vitamin A toxicity (hypervitaminosis A) from beta-carotene in plant foods. The BCMO1 enzyme that converts beta-carotene to retinol is downregulated when body stores are already adequate, creating a self-regulating safety mechanism. Excess unconverted beta-carotene is stored harmlessly in fat tissue and skin, sometimes causing a harmless orange-yellow skin tint called carotenodermia at very high intakes. This is cosmetic and reversible. Vitamin A toxicity is a risk only from high-dose preformed retinol supplements, which vegans do not typically use. This makes vegan vitamin A foods strategies inherently safer than omnivore supplementation approaches.
Do green smoothies provide meaningful vitamin A?
It depends entirely on the fat content of the smoothie. A green smoothie made with water, spinach, and banana contains meaningful beta-carotene but without fat present, most of it will not be absorbed. Adding nut butter, avocado, hemp seeds, or full-fat coconut milk (used sparingly) provides the fat matrix needed for carotenoid absorption. A green smoothie with a tablespoon of almond butter or half an avocado is a genuinely effective delivery vehicle for vegan vitamin A foods. The same smoothie without any fat source is not.
What are the early signs of vitamin A insufficiency on a vegan diet?
The earliest sign is night blindness, difficulty seeing in low-light conditions. Other early indicators include dry, rough skin with a sandpaper texture (follicular hyperkeratosis), dry eyes (xerophthalmia in more advanced cases), increased frequency of respiratory infections, and slow wound healing. Subclinical insufficiency may not produce obvious symptoms but can impair immune mucosal barriers and gut epithelial integrity in ways that manifest as increased susceptibility to infections or worsening digestive symptoms. If you suspect insufficiency, discuss serum retinol testing with a healthcare provider rather than self-supplementing, as the symptoms overlap with many other conditions.
Is the BCMO1 gene variant common and how does it affect vegan vitamin A?
The BCMO1 variants that reduce beta-carotene to retinol conversion are present in approximately 45% of the general population based on studies in European ancestry populations. Research suggests these variants reduce conversion efficiency by 32 to 69% compared to normal converters. For vegans, this means nearly half the population may need to consume substantially more beta-carotene from vegan vitamin A foods than standard recommendations suggest in order to achieve the same retinol activity. Consumer genetic tests do not currently provide reliable BCMO1 variant information. The practical response is to eat orange and green vegetables consistently, cooked with fat, and monitor vitamin A status periodically if you have risk factors.
Should pregnant vegans take a preformed vitamin A supplement?
Pregnant vegans should discuss vitamin A status specifically with their midwife, obstetrician, or registered dietitian. Vitamin A is critical for fetal development, and both deficiency and excess are harmful during pregnancy. The safe approach for pregnant vegans is to maximise dietary beta-carotene from vegan vitamin A foods, ensure fat is present at every relevant meal, and use a well-formulated vegan prenatal supplement that contains beta-carotene rather than preformed retinol as the vitamin A source. High-dose preformed vitamin A supplements are contraindicated in pregnancy. Food-based beta-carotene from plant sources does not carry toxicity risk and is the appropriate strategy for pregnant vegans.
How does vitamin A interact with other fat-soluble vitamins in a vegan diet?
The fat-soluble vitamins A, D, E, and K all compete for some of the same intestinal absorption pathways and transport mechanisms. Very high intakes of one can impair absorption of others. At dietary levels from whole vegan vitamin A foods, these interactions are not clinically significant. At supplemental doses, they become relevant: very high-dose vitamin A can antagonise vitamin D and K function. For vegans supplementing vitamin D, as most should, the combination with dietary beta-carotene from food presents no concern. The important principle is to obtain vitamin A from food rather than high-dose supplements, which avoids inter-nutrient competition while providing the full spectrum of carotenoids that beta-carotene-only supplements do not deliver.
Are orange-fleshed fruits meaningful vegan vitamin A foods?
Somewhat, but significantly less than orange and dark green vegetables. Mango provides approximately 54 mcg RAE per 100g. Cantaloupe provides approximately 169 mcg RAE per 100g. Apricot provides approximately 96 mcg RAE per 100g. These are meaningful contributions when eaten regularly and with fat, but they cannot substitute for sweet potato and carrot as primary vegan vitamin A foods. They work well as part of a diverse beta-carotene strategy rather than as standalone vitamin A sources. Papaya is worth noting specifically: approximately 47 mcg RAE per 100g, but it contains beta-cryptoxanthin as well as beta-carotene, adding carotenoid diversity to the diet.
Does vitamin A from vegan foods support skin health?
Yes, significantly. Retinoic acid (the gene-regulatory form of vitamin A) controls skin cell differentiation and proliferation. Adequate vitamin A maintains skin barrier function, supports sebaceous gland activity, reduces abnormal keratin accumulation, and supports the cell turnover rate that keeps skin smooth and clear. The same dietary beta-carotene that provides vitamin A also deposits in the skin as a direct antioxidant, protecting skin cells from UV damage independently of its vitamin A activity. The combination of internal vitamin A provision and topical carotenoid antioxidant protection makes vegan vitamin A foods among the most skin-relevant nutritional choices available. The skin nutrition framework on this site explores this in depth.
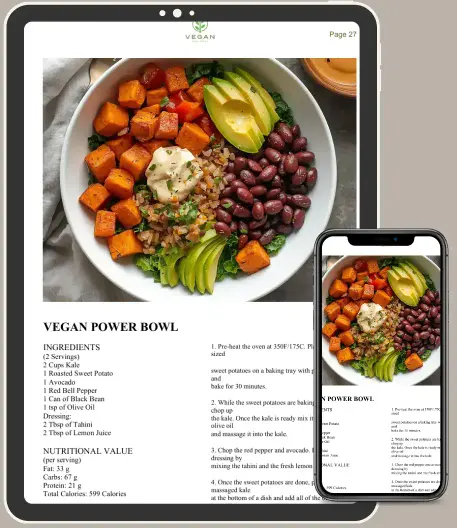
The Complete 28-Day Vegan Meal Plan + Grocery List
- 28-day structured calendar — breakfast, lunch, dinner & snack, every single day
- Every meal meets protein, iron & B12 — no guesswork, no gaps
- 4 weekly grocery lists — categorised, budget-friendly, zero waste
- Saves 7+ hours weekly — print once, follow all month
- Bonus Nutrition Guide Toolkit — vegan tips, guides & family meal prep
Instant digital download · Printable PDF · Use today
Conclusion: Building a Reliable Vegan Vitamin A Foods Strategy
Vegan vitamin A foods provide excellent beta-carotene that supports retinol synthesis, but they require intentional preparation and combination to deliver meaningful vitamin A activity. The two non-negotiable practices are cooking orange and green vegetables rather than relying on raw preparations for vitamin A, and always eating them with dietary fat. These two habits alone transform the vitamin A contribution of plant foods from marginal to substantial.
The conversion efficiency variability, the BCMO1 genetic factor, and the interaction with thyroid function and gut health mean that vitamin A is worth monitoring on a vegan diet rather than assuming adequate intake from colourful vegetables alone. Periodic blood testing for serum retinol, particularly during pregnancy, for those with thyroid conditions, and for those following very low-fat plant-based approaches, provides the reassurance that dietary strategy is translating into adequate vitamin A status.
With this as the final fat-soluble vitamin covered in the vegan nutrient pillar series, the full picture is now complete: vegan vitamin A foods (this guide), vitamin D, vitamin E, and vitamin K are all covered. Together, these four guides provide a complete fat-soluble vitamin nutrition framework for plant-based eating. Supporting research is available through PubMed, the NIH Office of Dietary Supplements at ods.od.nih.gov, and VeganHealth.org.