Medical Disclaimer: This article discusses dietary patterns and cancer risk based on published population research. It is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Cancer risk involves many factors beyond diet. If you are considering a vegan diet for cancer prevention alongside a cancer diagnosis or personal history, consult your oncologist before making dietary changes. This guide covers cancer risk reduction, not cancer treatment.
A vegan diet for cancer prevention is one of the most evidence-backed applications of plant-based nutrition. The American Institute for Cancer Research (AICR), the World Cancer Research Fund (WCRF), and the International Agency for Research on Cancer (IARC) have all identified diet as a significant modifiable cancer risk factor. Large prospective studies consistently show that people following plant-based dietary patterns have lower incidence of several major cancers.
This is important to say precisely and carefully. Diet is one factor among many in cancer risk. Genetics, age, environmental exposures, and chance all play roles that dietary choices cannot fully override. What the research shows is that a well-structured plant-based diet meaningfully shifts the odds, not eliminates risk, but shifts it in a favourable direction across a population of hundreds of thousands of people studied over decades.
This guide to a vegan diet for cancer prevention is built on that evidence. It does not overclaim. It does not promise outcomes. It gives you the mechanisms, the foods, and the protocol that align with the strongest available research on plant-based eating and cancer risk reduction.

-
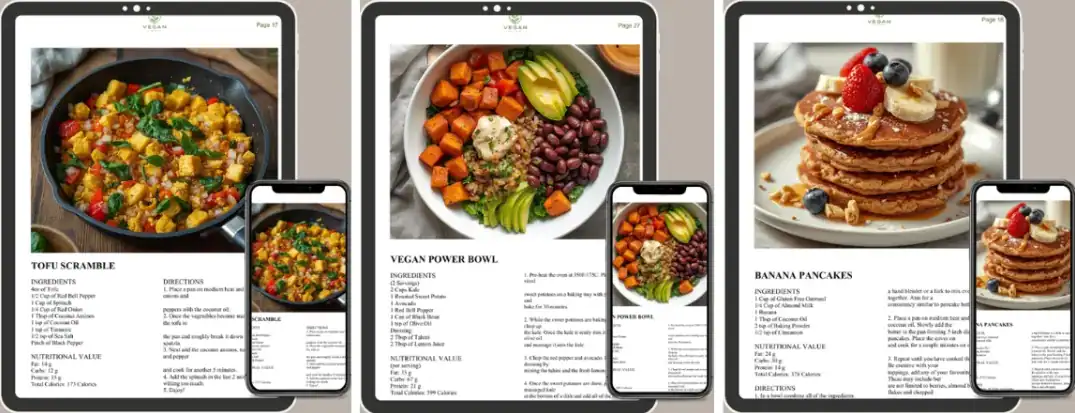
Complete 28-day calendarEvery breakfast, lunch, dinner & snack planned
-
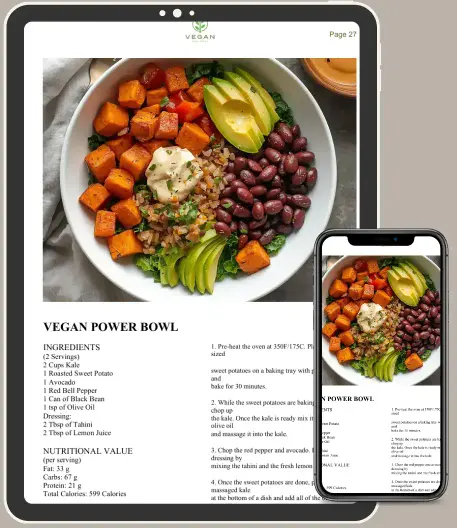
40+ nutritionist-approved recipesVibrant photo for every single dish
-
Easy weekly grocery listsShop smart, spend less, waste nothing
-
Protein, iron & B12 at every mealNutritionally complete — no guesswork
-
Saves 7+ hours weeklyPrint it once, follow it all month
-
Bonus: Nutrition Guide ToolkitVegan tips, guides & family meal prep
What the Evidence Actually Shows
The evidence base for a vegan diet for cancer prevention comes from multiple research streams across the past three decades. The most robust data comes from large prospective cohort studies and systematic reviews rather than short-term dietary intervention trials.
What the Studies Show, and What They Do Not
The strongest population evidence comes from the EPIC-Oxford study (65,000+ participants), the Adventist Health Study-2 (96,000+ participants), and a 2019 JAMA Internal Medicine meta-analysis of vegetarian and vegan cancer risk. All find meaningfully lower cancer incidence in plant-heavy dietary patterns.
Important caveat: These are observational studies. They show association, not definitive causation. People who follow plant-based diets also differ in other lifestyle factors including exercise, smoking rates, alcohol consumption, and body weight, all of which independently affect cancer risk. The dietary effect cannot be fully isolated. What the data does support is that consistent, whole-food plant-based eating is associated with a meaningfully lower cancer burden across large populations over long time periods.
A vegan diet for cancer prevention is best understood as one component of a broader risk-reduction lifestyle, not a standalone guarantee. That framing is both more accurate and ultimately more useful.

The Five Protective Mechanisms
The cancer-protective properties of a vegan diet for cancer prevention do not operate through a single pathway. Five distinct biological mechanisms contribute, and understanding each one clarifies which dietary choices matter most.
Processed meats (bacon, sausage, deli meats) are IARC Group 1 carcinogens: the same classification as tobacco smoke and asbestos. They are linked to colorectal and stomach cancer through nitrosamine formation during processing and cooking. A vegan diet eliminates this entire risk category by default.
The WCRF/AICR rates fibre intake as strong protective evidence for colorectal cancer, one of the highest evidence grades available. Fibre feeds bacteria that produce butyrate, a short-chain fatty acid that induces apoptosis in colon cancer cells and inhibits tumour growth in the colorectal epithelium. Vegans consistently consume two to three times more fibre than omnivores.
Plant foods contain thousands of biologically active compounds including polyphenols, carotenoids, glucosinolates, flavonoids, and lignans. These inhibit cancer development through multiple pathways: preventing DNA oxidation, modulating enzyme activity that activates carcinogens, and suppressing inflammatory signalling that promotes tumour microenvironments.
Insulin-like growth factor 1 (IGF-1) promotes cell proliferation and inhibits apoptosis, two processes central to cancer development. High animal protein intake, particularly dairy, raises circulating IGF-1 significantly. Multiple studies confirm vegans have 13% lower IGF-1 levels than omnivores, which is relevant particularly for breast, prostate, and colorectal cancer research.
Obesity is a confirmed risk factor for 13 distinct cancer types including breast, endometrial, colorectal, kidney, and pancreatic cancers. Excess adipose tissue elevates oestrogen, insulin, and systemic inflammation, all of which promote tumour development. Plant-based diets are consistently associated with lower BMI in population studies, making weight management an indirect but significant cancer-protective mechanism.
Note on mechanism strength: Mechanisms 1 and 2 have the strongest and most consistent human evidence. Mechanisms 3 and 4 have strong laboratory and some clinical evidence. Mechanism 5 is indirect but well-established. A diet that activates all five simultaneously, which a well-planned plant-based diet does, provides the broadest evidence-based coverage available from nutrition.
Top Anti-Cancer Plant Foods Ranked by Evidence Strength
The chart below ranks plant food categories by the strength and consistency of their cancer-protective evidence in a vegan diet for cancer prevention across human studies. Strong indicates consistent human prospective data. Moderate indicates human observational data with strong mechanistic support. Emerging indicates promising but less consistent human data.
Cancer-Protective Plant Food Categories: Evidence Strength
Source: WCRF/AICR Continuous Update Project; EPIC-Oxford; Adventist Health Study-2. Evidence ratings reflect consistency and quality of human prospective data.
8 Spotlight Foods: Mechanisms and Practical Use
These eight foods represent the strongest intersection of evidence strength, practical daily availability, and mechanistic understanding in the vegan diet for cancer prevention literature.
Foods Associated with Increased Cancer Risk
A vegan diet for cancer prevention has a significant structural advantage here: the foods with the strongest carcinogen associations are all animal-derived or ultra-processed. A whole-food plant-based diet eliminates or substantially reduces exposure to each of the following.
Vegan diet for cancer prevention advantage: A whole-food vegan diet automatically eliminates the top two risk categories (processed and red meat), avoids the animal fat that correlates with the hormone-driven cancers, and naturally reduces the energy density that drives obesity-linked cancer risk. Ultra-processed vegan foods are not exempt from the risk table above, plant-based burgers, vegan deli slices, and packaged convenience foods with long additive lists can replicate the ultra-processed food risk profile. Whole food matters as much as plant-based.
Cancer Type: Dietary Evidence Overview
The dietary evidence for a vegan diet for cancer prevention is not uniform across cancer types. The following summary reflects the current state of human prospective data for each cancer site most associated with plant-based dietary research.
Fibre, whole grains, and legumes have the strongest evidence of any dietary factors in any cancer prevention category. The WCRF/AICR rates dietary fibre as “convincing” evidence for colorectal cancer risk reduction. The elimination of processed meat is the most impactful single dietary change for this cancer type.
Plant-based diets are associated with lower circulating oestrogen (due to reduced adipose tissue and higher fibre intake that increases oestrogen excretion), lower IGF-1, and higher phytoestrogen intake from soy foods. Multiple studies associate high soy isoflavone intake with reduced breast cancer recurrence in post-menopausal women, contrary to earlier concerns. The evidence is favourable but more complex than colorectal.
Lower IGF-1 on vegan diets is the most direct mechanism. Lycopene from cooked tomatoes is associated with lower prostate cancer risk in several large prospective studies. High red meat and dairy intake is associated with higher risk via IGF-1 elevation. The elimination of these foods through plant-based eating creates a favourable prostate risk environment, though direct intervention trials remain limited.
High fruit and vegetable intake is consistently associated with lower risk of lung, oesophageal, stomach, and mouth/pharynx cancers across prospective studies. The carotenoid (beta-carotene, lycopene, lutein) and vitamin C content of a diverse plant diet is the primary mechanism. Notably, beta-carotene supplements increase lung cancer risk in smokers, this is an important caveat: the benefit is specific to whole food sources, not isolated supplements.
A diet centered on whole plant foods is rich in phytochemicals and fiber, which play a significant role in reducing the risk of certain chronic illnesses. According to the Harvard T.H. Chan School of Public Health, patterns emphasizing fruits, vegetables, and plant proteins are consistently linked to lower risk due to their ability to reduce inflammation. To further understand the impact of nutrition, the Cleveland Clinic recommends a high-fiber, low-fat diet rich in plant sources to protect cells and support the body’s natural defense mechanisms.
The 7-Step Vegan Cancer Prevention Protocol
This vegan diet for cancer prevention protocol is ordered by evidence strength. Steps 1 and 2 have the most robust human data. Steps 3-7 build on that foundation with strong mechanistic and observational support.
-
1Maximise fibre intake through legumes and whole grains daily
One cup of cooked legumes and three servings of whole grains per day delivers approximately 25-35g of dietary fibre, covering the WCRF target associated with the strongest colorectal cancer risk reduction. This is the single highest-evidence dietary intervention for cancer prevention available in the published literature. No supplement, superFood, or protocol comes close to the evidence strength behind sustained high-fibre whole-food plant intake.
-
2Eat at least five portions of non-starchy vegetables and fruit daily
This is the WCRF/AICR baseline recommendation. Include at least one cruciferous vegetable and one allium (garlic or onion) in this five-a-day minimum. Variety matters: different plant foods provide different phytochemical classes that operate through distinct anti-cancer pathways. A plate with five different vegetable colours typically covers five different phytochemical families. See the anti-inflammatory plant diet guide for the full colour-nutrient guide.
-
3Eliminate ultra-processed foods, including ultra-processed vegan alternatives
Replacing whole food meals with ultra-processed plant-based convenience products does not replicate the cancer-protective effect of whole plant foods. A 2022 BMJ study found that every 10% increase in ultra-processed food consumption was associated with a 10% higher cancer risk, regardless of dietary pattern. Whole foods, not dietary labels, determine cancer risk outcomes. The gut health guide covers the microbiome impact of ultra-processed foods.
-
4Include cruciferous vegetables at least five times per week
Broccoli, kale, cauliflower, Brussels sprouts, cabbage, and bok choy. Lightly steam or eat raw to preserve glucosinolate content. Chew thoroughly, the myrosinase enzyme that activates glucosinolates into sulforaphane is released by chewing. Well-chewed, lightly steamed broccoli delivers more sulforaphane than heavily boiled broccoli that has been minimally chewed.
-
5Maintain a healthy body weight through calorie-appropriate whole food eating
Obesity is a confirmed causal risk factor for 13 cancer types. A whole-food plant-based diet, with its high fibre content, high water content, and lower energy density, supports weight management more effectively than any other dietary pattern in meta-analyses. This is an indirect but powerful cancer-prevention mechanism. Maintaining a healthy BMI (18.5-24.9) through whole-food plant eating reduces the oestrogen, insulin, and inflammatory signalling that adipose tissue produces.
-
6Add fermented plant foods to support the gut microbiome
A diverse, butyrate-producing gut microbiome is one of the most important mechanisms behind fibre’s cancer protection. Fermented plant foods, sauerkraut, kimchi, miso, and tempeh, introduce beneficial bacteria that support butyrate production while also providing prebiotic organic acids. The 2021 Stanford Cell study found high fermented food intake reduced 19 inflammatory proteins, including several implicated in tumour microenvironment formation.
-
7Avoid alcohol and attend recommended cancer screening
Alcohol is an IARC Group 1 carcinogen for six cancer types, with no safe lower threshold confirmed. Even modest alcohol consumption increases breast cancer risk in women. Diet and lifestyle are complementary to, not substitutes for, regular cancer screening programmes. A vegan diet for cancer prevention has the greatest impact when combined with screening attendance, non-smoking, and physical activity as a complete risk-reduction approach rather than a standalone dietary strategy.
A Chef’s Perspective: MENA Spice and Herb Traditions in Cancer Research
In over 20 years cooking professionally across the Middle East and Mediterranean, I worked daily with ingredients that cancer researchers are now studying intensively. Turmeric, black pepper, garlic, cumin, coriander, saffron, and sumac were not considered health foods in the professional kitchens I worked in. They were flavour. That they also carry meaningful biological activity is something nutritional science has confirmed in retrospect.
The MENA cooking tradition builds alliums into every savoury base, garlic and onion are non-negotiable in Lebanese, Gulf, and North African cooking. Every rice dish, every stew, every sauce begins with this combination. The allicin and quercetin load in a traditional MENA diet is substantially higher than in Western dietary patterns, and this aligns well with the WCRF evidence on stomach and colorectal cancer risk.
Turmeric used daily in dhal, rice dishes, and marinades compounds its cancer-protective potential over years and decades of consistent use. The dose in cooking, a teaspoon per meal, several times weekly, is lower than in most clinical trials, but the consistent lifetime exposure from culinary tradition may be more relevant than the short-term supplemental doses studied in trials.
My practical advice: cook with spices deliberately, not decoratively. Build turmeric and black pepper into every lentil dish. Use garlic generously in every savoury base. Cook tomatoes in olive oil rather than serving them raw for maximum lycopene. These are not significant departures from how most people already cook. They are small adjustments that consistently apply the anti-cancer plant principles supported by the best available evidence. The Ultimate 28-Day Vegan Meal Plan + Grocery List (Complete Solution) is built on this philosophy: 36 chef-tested whole-food recipes with a photo for every recipe, using common supermarket ingredients, with every meal meeting protein, iron, and B12 needs.
28-Day Vegan Meal Plan
+ Grocery List
Complete Solution · Nutritionist-Approved · Print & Use Today
Read on any device · No apps needed
Frequently Asked Questions
Can a vegan diet prevent cancer?
No dietary pattern can guarantee cancer prevention, and it is important to be clear about this. What the evidence shows is that people following plant-based dietary patterns have statistically lower cancer incidence in large population studies. A well-planned vegan diet for cancer prevention meaningfully shifts cancer risk in a favourable direction by eliminating the most carcinogenic foods, maximising protective plant compounds, and supporting healthy weight. The effect is probabilistic and population-level, not individual and absolute.
Which cancers have the strongest evidence for dietary prevention?
Colorectal cancer has the strongest and most consistent dietary evidence. The WCRF/AICR rates fibre intake as “convincing” protective evidence and processed meat as “convincing” risk evidence, the highest rating available. Stomach cancer and oesophageal cancer also have strong associations with plant food intake. Breast and prostate cancer have moderate evidence. All cancer prevention dietary research supports the same broad principles: more whole plant foods, less processed and animal food.
Is soy safe for breast cancer survivors?
Current evidence supports the safety of moderate soy consumption for breast cancer survivors, including those with hormone-receptor-positive cancers. Multiple large prospective studies, including a Shanghai Women’s Health Study analysis, found that higher soy intake was associated with reduced breast cancer recurrence and mortality. The earlier concern about soy phytoestrogens was based on laboratory studies using isolated isoflavones at non-dietary doses. Whole soy foods at dietary amounts (edamame, tofu, tempeh) are considered safe by major oncology organisations. Always discuss with your oncologist for individual guidance.
Does eating organic produce significantly reduce cancer risk?
The evidence for organic produce and cancer risk reduction is weak and inconsistent in human studies. The NutriNet-Santé cohort (70,000+ French adults) found some association between organic consumption and lower overall cancer risk, but the effect was modest and confounded by multiple healthy lifestyle factors among organic consumers. The cancer-protective evidence for plant foods, organic or conventional, overwhelmingly points to increasing the quantity and variety of plant foods as the primary driver, not organic status. Do not let the cost of organic produce reduce your total vegetable and fruit consumption.
Are there anti-cancer supplements worth taking on a vegan diet?
With very few exceptions, isolated anti-cancer supplement trials have been disappointing or harmful. High-dose beta-carotene supplements increased lung cancer risk in smokers in the CARET and ATBC trials. High-dose vitamin E supplementation increased prostate cancer risk in the SELECT trial. The cancer-protective compounds in plants appear to work through complex whole-food matrices and synergistic interactions, not in isolation at high doses. The important exception is vitamin D, where adequate status (40-60 ng/mL) is associated with lower cancer incidence across multiple studies, and supplementation is appropriate for vegans to ensure adequacy.
How important is fibre specifically for cancer prevention?
Fibre is the most evidenced single dietary component for cancer prevention in human data. The WCRF/AICR rates whole grain fibre and dietary fibre as “convincing” protective evidence for colorectal cancer, the highest rating in their evidence grading system. The mechanism operates through transit time reduction, butyrate production, and the reduction of bile acid concentration in the colon. A vegan diet built around legumes, whole grains, and vegetables typically delivers 30-40g of fibre per day versus the average Western diet’s 15g, making this one of the most meaningful structural differences in cancer risk profile between the two patterns.
Does cooking method affect the cancer-protective compounds in vegetables?
Yes. Boiling leaches water-soluble phytochemicals into cooking water. Steaming, roasting, stir-frying, and microwaving preserve significantly more anti-cancer compounds. For cruciferous vegetables specifically, light steaming or raw consumption preserves glucosinolates better than boiling. Cooking tomatoes in oil dramatically increases lycopene bioavailability. Crushing garlic and allowing it to rest before cooking maximises allicin. The practical principle: use minimal water, moderate heat, and incorporate cooking liquid into final dishes wherever possible.
Does a plant-based diet help during cancer treatment?
This guide addresses cancer risk reduction, not cancer treatment. During active cancer treatment, nutritional needs change significantly depending on the treatment type, cancer site, and individual medical situation. Maintaining adequate protein, calorie intake, and specific micronutrient levels is critical during treatment. If you have a cancer diagnosis, dietary decisions during treatment should be made with your oncologist and a registered dietitian specialised in oncology nutrition. Do not follow a cancer prevention dietary protocol as a treatment strategy without medical supervision.
What is the WCRF/AICR cancer prevention framework?
The World Cancer Research Fund (WCRF) and American Institute for Cancer Research (AICR) produce the most comprehensive systematic reviews of cancer and lifestyle evidence available. Their 2018 Third Expert Report and ongoing Continuous Update Project grade dietary associations as “convincing,” “probable,” “limited” or “no conclusion.” Their dietary recommendations align closely with a vegan diet for cancer prevention approach: be a healthy weight, be physically active, eat a diet rich in whole grains, vegetables, fruit, and legumes, limit red meat, avoid processed meat and alcohol. A vegan diet for cancer prevention addresses every single item on that list by its structural nature.
Is whole food more important than plant-based for cancer prevention?
Both matter, and they are not interchangeable. A whole-food omnivorous diet with high vegetable and fibre intake likely outperforms a junk-food vegan diet for cancer risk. A whole-food vegan diet for cancer prevention likely outperforms both because it combines the whole-food advantage with the processed meat elimination advantage. The evidence base is for plant-based whole food eating, not plant-based eating broadly defined. Ultra-processed vegan convenience foods do not carry the cancer-protective properties of whole legumes, vegetables, and grains.
How long does it take for dietary changes to affect cancer risk?
Cancer develops over years to decades. The dietary evidence is based on long-term habitual patterns, not short-term interventions. That said, some mechanisms are relatively rapid: the gut microbiome shifts meaningfully within weeks of a dietary change, inflammation markers respond within months, and IGF-1 levels adjust within weeks of protein and dietary pattern changes. The full cancer risk benefit of a vegan diet for cancer prevention accumulates over years of consistent eating. Starting sooner is substantially more valuable than starting later, but there is meaningful benefit at any age from adopting a more protective dietary pattern.
What is the role of vitamin C in cancer prevention?
Vitamin C has two specific cancer-prevention roles in the dietary evidence. First, it is a potent antioxidant that prevents the formation of carcinogenic N-nitroso compounds in the stomach, directly blocking one of the mechanisms by which processed meat increases stomach and colorectal cancer risk. Second, high-vitamin-C plant food intake is consistently associated with lower risk of oesophageal and stomach cancers in prospective studies. The vegan vitamin C guide covers the best plant sources and how to maximise daily intake.
A Plant-Based Diet and Cancer Risk: The Evidence in Summary
The evidence for a vegan diet for cancer prevention is substantial, nuanced, and worth understanding precisely. The mechanisms are real, fibre and the gut microbiome, processed meat elimination, phytochemical activity, lower IGF-1, and weight management all contribute meaningfully to a lower cancer risk profile. The limitations are also real: observational data cannot establish absolute causal certainty, and diet is one factor in a multi-factorial risk picture.
What the evidence supports clearly: whole grains and legumes daily for fibre, cruciferous vegetables regularly for glucosinolates, colourful fruit and vegetables for polyphenols, eliminating ultra-processed foods, and maintaining a healthy body weight. A well-planned plant-based diet delivers all five simultaneously through its basic structural logic.
If you want a practical, structured foundation for eating this way consistently, the Ultimate 28-Day Vegan Meal Plan + Grocery List (Complete Solution) gives you 36 chef-tested whole-food recipes with a photo for every recipe, four weekly grocery lists, and a complete 28-day calendar. Every meal is built from simple supermarket ingredients and meets protein, iron, and B12 needs. It is a structured starting point for the kind of consistent, whole-food plant-based eating that the cancer prevention evidence is built on, not a medical intervention, but a practical system for eating well.